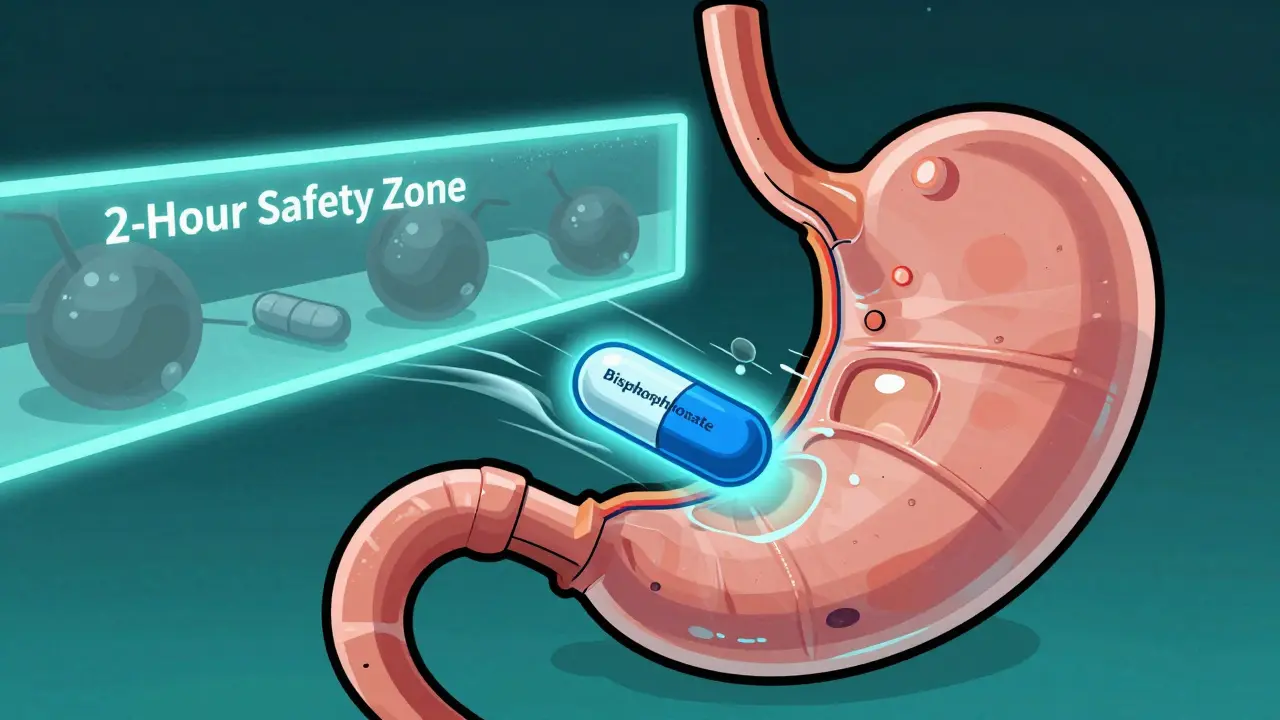
You might think taking a magnesium supplement alongside your osteoporosis medication is harmless. After all, both are meant to support your health. But this common habit could be silently undoing months of treatment. For millions of people managing osteoporosis, a condition that weakens bones and increases fracture risk, the effectiveness of their prescription drugs depends entirely on how they handle over-the-counter supplements. Specifically, the interaction between magnesium and oral bisphosphonates is not just a minor footnote in a drug guide-it is a critical factor that determines whether your bones get stronger or stay vulnerable.
If you are taking medications like alendronate (Fosamax) or risedronate (Actonel), you need to know exactly when to take your magnesium. Getting the timing wrong can reduce the absorption of your osteoporosis drug by up to 60%. This isn't about being overly cautious; it is about ensuring the medicine actually reaches your bloodstream. In this guide, we will break down the science behind this interaction, provide a step-by-step schedule you can follow today, and help you identify hidden sources of magnesium that might be sabotaging your treatment.
Why Magnesium Blocks Your Osteoporosis Medication
To understand why timing matters, we have to look at what happens inside your stomach. Oral bisphosphonates are a class of drugs designed to slow down bone loss. They work by inhibiting osteoclasts, the cells responsible for breaking down bone tissue. However, these drugs are notoriously difficult for the body to absorb. Under perfect conditions, your body absorbs only 0.6% to 12% of the dose you swallow. That is why doctors instruct you to take them on an empty stomach with plain water and remain upright for 30 minutes.
Magnesium interferes with this already fragile process through a chemical reaction called chelation. When magnesium ions meet the phosphonate groups in your medication, they bind together to form insoluble complexes. Think of it like trying to dissolve sugar in oil-the mixture simply doesn't work. These clumps cannot pass through the intestinal wall into your bloodstream. Instead, they pass right through your system unused. According to pharmacokinetic studies cited by the FDA, co-administering magnesium can cut the absorption of alendronate by 40% to 60%. If your baseline absorption was already low, this drop can render the medication clinically ineffective.
This interaction affects all major oral bisphosphonates, including:
- Alendronate (brand names Fosamax, Binosto)
- Risedronate (brand names Actonel, Atelvia)
- Ibandronate (brand name Boniva)
Note that intravenous formulations, such as zoledronic acid (Reclast), bypass the gastrointestinal tract entirely. If you receive your medication via infusion, magnesium timing is less critical because the drug enters your blood directly. However, if you are popping pills, the rules below are non-negotiable.
The Golden Rule: The Two-Hour Window
The medical consensus is clear and consistent across major health organizations. You must separate the intake of oral bisphosphonates and magnesium by at least two hours. This recommendation comes from the National Institutes of Health Office of Dietary Supplements, WebMD Drug Database, and clinical reviews published in journals like the Journal of Bone and Mineral Research.
Why two hours? It takes roughly that long for your stomach to empty its contents into the small intestine, where most drug absorption occurs. By waiting two hours, you ensure that the bisphosphonate has moved past the primary zone where magnesium would interfere with it. Some guidelines suggest even longer gaps for extended-release formulations, but two hours is the universal minimum standard for immediate-release tablets.
| Medication Type | Interaction Risk | Required Separation Time | Notes |
|---|---|---|---|
| Oral Bisphosphonates (Alendronate, Risedronate, Ibandronate) | High | At least 2 hours | Takes bisphosphonate first, wait 2+ hours before magnesium |
| Intravenous Bisphosphonates (Zoledronic Acid) | Low/N/A | No strict timing needed | Bypasses gut absorption |
| Denosumab (Prolia) | Low | No strict timing needed | Injectable, different mechanism |
| Calcium Supplements | High | At least 2-4 hours | Similar chelation effect as magnesium |
Dr. Felicia Cosman, clinical director of the National Osteoporosis Foundation, has noted that non-adherence to dosing protocols is the single largest preventable cause of treatment failure. Ignoring this two-hour window puts you in that high-risk category. Studies show that patients who properly separate these medications achieve significantly better improvements in bone mineral density compared to those who do not.
Hidden Sources of Magnesium You Might Be Missing
Most people realize they are taking magnesium if they see a bottle labeled "Magnesium Citrate" or "Magnesium Glycinate." But magnesium hides in many other products you might use daily without thinking twice. If you take any of these within two hours of your osteoporosis pill, you risk reducing its efficacy.
Antacids: Many popular antacids contain magnesium hydroxide or magnesium carbonate. Brands like Maalox, Mylanta, and Milk of Magnesia are heavy hitters here. A single dose of Milk of Magnesia can contain up to 800mg of magnesium. Even occasional use for heartburn can disrupt your medication schedule if timed poorly.
Laxatives: Similar to antacids, some laxatives use magnesium to draw water into the intestines. Check the active ingredients list for "magnesium oxide" or "magnesium citrate."
Electrolyte Drinks and Bottled Water: Some sports drinks and naturally mineralized waters, such as San Pellegrino, contain significant amounts of magnesium. While usually lower than supplement doses, frequent consumption close to your medication time adds up.
Multivitamins: Most standard multivitamins include magnesium. If you take a morning multivitamin with your breakfast, and then take your bisphosphonate later, or vice versa, you need to ensure there is a sufficient gap. Ideally, take your bisphosphonate well before your multivitamin.
A survey by the National Osteoporosis Foundation found that 37% of patients taking both magnesium and bisphosphonates were unaware of this interaction. Another 22% admitted to taking them simultaneously. Being proactive means auditing every product that goes into your mouth, not just your prescription bottles.

A Practical Daily Schedule for Success
Knowing the rule is one thing; living it is another. Integrating strict timing into a busy morning routine can be challenging, especially if you manage multiple medications. Here is a practical, step-by-step protocol recommended by geriatric specialists to maximize adherence.
- Wake Up and Take Bisphosphonate: As soon as you wake up, take your oral bisphosphonate with a full glass (8 oz) of plain water. Do not use coffee, juice, or mineral water. Stay upright (sitting or standing) for at least 30 minutes. Do not eat anything during this time.
- The Waiting Period: Set a timer for 30 minutes. Once that is done, you can have your breakfast. However, do not take any magnesium-containing supplements yet. Continue to wait until a total of two hours have passed since taking the bisphosphonate.
- Take Magnesium: After the two-hour mark, you can safely take your magnesium supplement. This is also a good time to take calcium supplements, as they have similar interaction risks with bisphosphonates.
- Document It: Use a medication log or a specialized pill organizer with AM/PM compartments. Standard weekly boxes often fail because they don't account for intra-day timing. Visual aids, like a "timing wheel" sticker on your fridge, can help reinforce the routine.
If you prefer taking magnesium in the evening for sleep support, that works too-just ensure you took your bisphosphonate at least two hours earlier. The key is consistency. Whether you choose morning or evening for magnesium, stick to it so your body and routine adapt.
What Happens If You Mess Up?
Let's say you accidentally took your magnesium and bisphosphonate at the same time. Should you panic? Not necessarily. One instance won't destroy your bone density overnight. However, making this a habit will. Chronic under-dosing leads to accelerated bone loss and increased fracture risk. Real-world reports from patient communities highlight stories of individuals who suffered fractures despite being "on treatment," only to discover later they had been neutralizing their medication with antacids or supplements.
If you miss the window, do not double up on your bisphosphonate the next day unless instructed by your doctor. Simply resume your normal schedule. If you frequently struggle with timing, talk to your healthcare provider. There may be alternative treatments, such as injectable denosumab (Prolia) or teriparatide (Forteo), which do not have these specific gastrointestinal interactions. Additionally, new time-release formulations are in development that aim to reduce susceptibility to mineral interactions.
Remember, osteoporosis management is a long game. Small errors in daily habits compound over years. By mastering the timing of your magnesium and osteoporosis medications, you protect the investment you are making in your skeletal health. Your bones rely on getting the full dose of protection they need-make sure they get it.
Can I take magnesium and alendronate (Fosamax) at the same time?
No, you should not take them at the same time. Magnesium binds to alendronate in the stomach, forming insoluble complexes that your body cannot absorb. This can reduce the effectiveness of alendronate by 40-60%. You must wait at least two hours after taking alendronate before consuming magnesium.
Does food affect the interaction between magnesium and osteoporosis meds?
Yes, food plays a role. Oral bisphosphonates must be taken on an empty stomach with plain water, and you must wait 30 minutes before eating. Since magnesium is often found in foods and supplements, keeping your stomach empty initially helps ensure the bisphosphonate moves through quickly. Eating magnesium-rich foods immediately after your 30-minute wait is generally safer than taking a concentrated magnesium supplement, but a 2-hour gap is still the safest protocol.
Which magnesium supplements interact with bisphosphonates?
All forms of magnesium supplements can interact with oral bisphosphonates, including magnesium citrate, magnesium glycinate, magnesium oxide, and magnesium chloride. The interaction is due to the magnesium ion itself, regardless of the compound it is attached to. Therefore, the 2-hour separation rule applies to all types.
Do I need to separate magnesium from Denosumab (Prolia)?
No, strict timing separation is not required for Denosumab (Prolia). Unlike oral bisphosphonates, Denosumab is an injectable medication administered every six months. It does not pass through the digestive system, so it is not affected by dietary magnesium or supplements taken orally.
What if I take magnesium for restless leg syndrome at night?
If you take your bisphosphonate in the morning, taking magnesium at night is perfectly fine and often easier to manage. Just ensure that at least two hours have passed since your morning dose. Since you likely won't be eating or drinking much before bed, this creates a natural buffer zone that minimizes interaction risks.
Can antacids like Tums or Maalox interfere with osteoporosis medication?
Yes, especially those containing magnesium or calcium. Antacids like Maalox, Mylanta, and Milk of Magnesia contain high levels of magnesium. Calcium-based antacids like Tums also interact with bisphosphonates. You should avoid taking any antacid within two hours of your osteoporosis medication. If you have chronic heartburn, discuss alternative timing strategies or medications with your doctor.